Does induced abortion affect future fertility and pregnancy complications? This question often cannot be answered without individuals, perhaps even inadvertently, wading into political commentary on abortion. Answers are often clouded by political agendas and funding sources, and co-opted and spun by either side of the abortion debate to push their own narrative.
On the pro-life side, I’ve sometimes seen the affects of abortion on fertility talked about like a horror story, showcasing a uterine perforation or the need for a hysterectomy because of a botched abortion, with nary a citation to help understand how often these outcomes happen. I’ve also experienced pro-life people unable to explain how, exactly, abortion can effect fertility. Talking about how bad abortion is for women can come across as a fear-mongering tactic in these kinds of situations and can make pro-life people seem ignorant.
On the other side, you have pro-choice people who will outright deny abortion does any harm at all to women’s fertility or that it can affect future pregnancies. You’ll see them hail how safe abortion is and how rare complications are, often with a decontextualized citation, or claim that it’s irrelevant because abortion is safer than childbirth (which isn’t true, by the way). They can come across as blasé in their total denial, making abortion sound too good to be true.
So…should we care about the answer to this question? What is the answer, and what should be done about it?
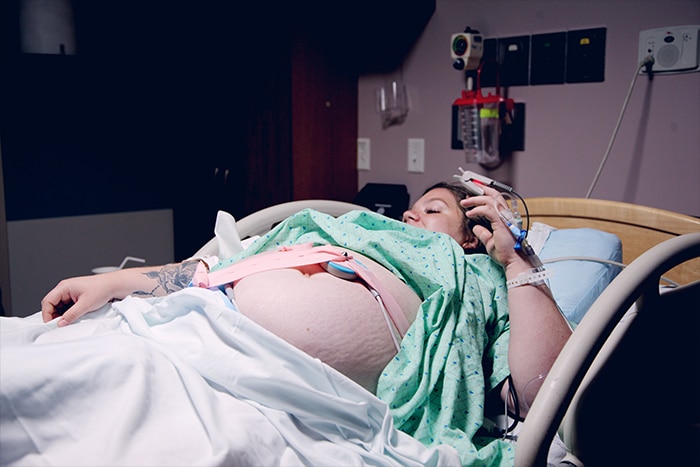
Estimated reading time: 12 minutes
Should we care?
Before I share my own views on the answer to this question, I posed a version of this question on Twitter and to people in other social circles I am in:
Why should both #ProLife and #ProChoice people care about whether #abortion affects future pregnancies and/or fertility?
Or even, should they care at all?
Does the answer matter?
Why/not?
Here were some of the replies:
-
we should all care about what happens to women in reproduction including:
– whether they had informed consent on the potential issues
– how the abortion experience impacts pregnancy, birth, and parenting mentally and emotionally
– how women see future struggles with infertility (pro-life person)
-
As someone who was 100% certain I never wanted children in my 20s, I wasn’t at all concerned about my fertility. Having done a complete 180 in my early 30s, IMO everyone should be concerned about how abortion affects their fertility. Minds can and do change. (pro-life person)
-
…pro-choicers and pro-lifers should both be equally concerned about informed consent. A woman should know truth & side effects of any decision she undergoes. (pro-life person)
-
Abortion rarely causes any adverse effects to future fertility….no, they shouldn’t focus on fertility issues, because fertility issues are rare! Miscarriages and childbirth complications and deaths are much more dangerous, and occur more often, than having a medical abortion! (pro-choice person)
-
Why don’t you directly ask women who have had abortions, miscarriages, that suffer from the consequences mentally and physically your obvious question? I’m sure both pro life and pro choice agree a women has a right to a safe pregnancy and the option to become pregnant naturally. (pro-choice person)
While I cannot claim the type of replies I got from either side are representative of either movement as a whole, I found it striking the pro-choice people’s responses were so dismissive of the question and the pro-life people’s responses seemed to be in favor of “informed consent.”
Now, maybe it’s a bias on the part of pro-lifers—perhaps they only want informed consent of possible outcomes of abortion if the outcomes are negative, to dissuade women from getting an abortion. But I intentionally included no studies or data in my question or in any of my responses to anyone; I did not want to confirm or deny whether abortion affected future fertility or pregnancy outcomes, because I did not want to influence people’s responses with the data.
Does Abortion Affect Future Female Fertility and Pregnancy Outcomes?
So….what does the data say?
In short: usually one abortion will not affect chances of carrying to term or having complications during pregnancy; but having multiple abortions can. Any single abortion can increase the risk of developing Asherman syndrome or Pelvic Inflammatory Disease, either of which can lead to fertility issues. These complications can be caused directly by the abortion or by conditions or infections to which abortion makes one more susceptible.
When attempting to answer this question, I looked at a few things. First, I looked at what might cause infertility in women. I did this because a study may not frame a research aim or report results as investigating the correlation, if any, between induced abortion and infertilty or pregnancy complications. However, a study may do those things for a correlation between induced abortion and a single risk factor for infertility and pregnancy complications.
I then searched for peer-reviewed journal articles which had robust populations (to cut down on selection bias), and preferably were case-controlled (so there was a control population of women to compare to) and had at least some incorporation of medical records (to reduce the chance of bias in self-reporting medical events in the past and self-reporting current complications). This unfortunately means not many US studies are considered. European countries are much better at being able to have both robust populations and medical record-linked studies.
Authors, even of peer-reviewed, published medical and scientific studies, can of course be biased. I strived to use studies no matter the author’s known pro-life or pro-choice stance if the methodolgy of the study seemed to cut down on selection bias and reporting bias and used statistical models which were able to give results adjusted for confounding factors. If a correlation exists between induced abortion and risk factors for infertilty or pregnancy complications, those should exist whether the authors are biased or not, if their study methods are rigorous.
How PID from Abortions Leads to Infertility
One common risk factor for infertility is Pelvic Inflammatory Disease (PID), which is caused by inflammation from an infection which has travelled from the vagina or cervix and infected the uterus, fallopian tubes, and/or ovaries. PID can cause scarring in the fallopian tubes which can inhibit both egg and sperm movement, can prevent fertilization from ever happening, or cause an ectopic pregnancy if fertilization does happen. PID can also cause damage to other parts of a woman’s reproductive tract, from her ovaries to her uterus.
About one in every 23 women in her lifetime will get PID (4.4%), and over one million women per year in the US are diagnosed with PID. However, it is thought that PID is under-diagnosed because the symptoms may not be so bad as to be interpreted as a problem until they get really bad. In fact, many women may not realize they have PID until they try to have a child and cannot. About 8% of women suffer enough tubal damage from one episode of PID to become infertile. After three episodes of PID, the infertility rate reaches 40%. If you get it once, you’re more likely to get it again, and then the more likely you are to become infertile. It’s a vicious cycle.
Any sexually active woman is at risk for PID, though women age 25 or younger are most at risk. PID is most common among women who have an STI, who have had multiple sexual partners, who have a partner who has had multiple sexual partners, and/or who have had a previous diagnosis of PID. STIs like chlamydia, a common infection leading to PID, are more common in younger women: for chlamydia, more than half of all infections involve people ages 18 to 24.
This is significant because 37% of abortions in 2018 (the most recent year for abortion stats) were on women 24 years old or younger. These younger women getting abortions are the same ones most likely to have the STIs leading to PID, and they’re the most at risk for PID in general.
Abortion inherently carries a risk of PID because it involves either inserting something into the vagina, through the cervix, and into the uterus, thereby possibly bringing a vaginal infection up further into the reproductive tract; or it involves cervix-softening drugs (both mifepristone and misoprostol) which can make it easier for infections to travel through the cervix.
Studies from Norway, Sweden, and India spanning decades of research and citing numerous other studies have shown:
- Women are at risk for PID after an abortion, whether surgical or medical
- Having an infection like Chlamydia or M. genitalium at the time of an abortion increases the chances of PID further
- Routine prophylactic antibiotics may or may not reduce chances of PID, depending on other confounding factors
The Indian study in particular also found miscarriage carried a risk for PID.
Even studies produced by pro-choice authors with affiliations to pro-choice groups like the Society of Family Planning, World Health Organization, and International Federation of Abortion and Contraception Professionals acknowledge here, here, and here respectively that there is a risk of developing PID after induced abortion, which is why STI screening, prophylactic antibiotic use, and use of sterile instrumentation is emphasized by the authors of these stuides. A 2011 literature review of postabortal PID confirmed that younger women, women who had STIs at the time of their abortion, and a previous PID dignosis were at higher risk of developing PID after an induced abortion, whether surgical or medical.
PID, Asherman Syndrome, and Infertility
Uterine scarring from PID or from curettage can also lead to a specific condition, Asherman Syndrome, which affects fertility. Scarring and/or excess tissue in the uterus involved in Asherman Syndrome can prevent implantation of an embryo and can cause a higher risk for miscarriage (death after implantation). Interestingly, while the Mayo Clinic says women who have multiple surgical abortions can get Asherman Syndrome, the actual papers on Asherman Syndrome say the risk is there, even after the first surgical abortion:
“It may occur in up to 13% of women undergoing a termination of pregnancy during the first trimester, and 30% in women undergoing a dilation and curettage (D and C) after a late spontaneous abortion.The risk increases for patients undergoing repeated procedures for bleeding or repeated elective termination of pregnancies.”
Other studies have found that the chance of Asherman Syndrome could range from 10% to 40% after a curettage, no matter the reason for the curettage (induced abortion, miscarriage treatment, post-pregnancy, etc.).
Another cause for infertility can include damage to fallopian tubes (tubal infertility), which can come not only from PID, but also from previous abdominal or pelvic surgery, including surgery for ectopic pregnancy. Scar tissue in the tubes can prevent fertilization and can prevent proper implantation, leading to no pregnancy or an increased risk for ectopic pregnancy.
Because data shows that induced abortion increases the chances of PID, or scarring of the reproductive tract independent of PID, then logically we can conclude that induced abortion leads to increased chance of infertility.
Ectopic Pregnancy
Research on whether induced abortion can increase the risk of ectopic pregnancy is mixed but suggests it certainly is possible. PID can increase the chance of ectopic pregnancy by over six times compared to a woman who has not had PID. Since an induced abortion can put a woman at higher risk for PID, it could, as a secondary affect, increase a woman’s chance of ectopic pregnancy.
A couple of large studies from France have found that induced abortion may increase the risk of ectopic pregnancy, with the chance for ectopic pregnancy becoming higher with increasing number of induced abortions. This was true for both medical and surgical abortions.
Pregnancy Complications
Some large European studies have been done investigating the risk factors of various pregnancy complications and they all show a correlation to induced abortion.
For example, studies from France (1995 and 1997), Australia, Finland, Scotland, and a 10-European-country survey have all shown a correlation between number of previous induced abortions and increased risk of preterm birth. And this is just the tip of the iceberg. Most of these studies cite numerous others done showing this same correlation. Usually two or more previous induced abortions is correclated with about a twice as high risk of preterm birth.
Literature reviews have also found a consistent positive correlation between induced abortion and chance for preterm birth, as well as other pregnancy complications such as placenta previa and preterm premature rupture of membranes (PPROM).
The authors of theses studies generally recognize two reasons for this correlation: the mechanics of induced abortion and the risk of infection after an abortion. Mechanically, opening the cervix and suctioning/scraping the uterus can lead to damage to the cervix and/or uterus and cause pregnancy complications such as placenta previa, which can be a cause of preterm birth. Preterm rupture of membranes (PROM) and PPROM are other reasons for preterm delivery and can be due to an upper genital tract infection, which we already have seen can happen after an abortion.
We Should Care About How Medical Decisions Affect Future Fertility
There is more than enough evidence to reasonably conclude that abortion can affect future pregnancies and women’s fertility.
The risks of some of these adverse outcomes, like PID, infertility, and preterm birth, may be small enough that a woman does not care about them and would still choose to have an abortion. However, many women who get abortions may want to have a child or multiple children later in life, and these women may decide the possible cost of a first, second, or third abortion is too high and outweighs the perceived benefit of the abortion. As long as abortion is legal, shouldn’t women be able perform a cost-benefit analysis and come to an informed decision about not only their current pregnancy, but also their future reproductive health?
For all that abortion advocates cry out for abortion to be recognized as a totally normal medical procedure, nothing to be ashamed of, essential health care, etc., they seem to resist any regulation of abortion as a normal surgical or medical procedure. Parental consent for minors, transfer agreements with hospitals like any other similar standalone medical clinic, informed consent, waiting periods—these are all seen as unnecessary barriers to abortion access. But these are all regulations that any other medical practice performing normal and essential healthcare services would have to abide by. Would we as a nation be disagreeing over informed consent for any other “normal medical procedure”? For example, if tonsillectomies were shown to increase the chance of throat cancer by two to three times that of a person who never had a tonsillectomy, would there be an outrage over whether people getting a tonsillectomy were required to be told that piece of information?
I would dare say the majority of both pro-life and pro-choice people genuinely care about the well-being of women and want women to be able to make medical decisions based on accurate information. It seems reasonable to say people on both sides of the abortion debate should, for the sake of women’s health and our autonomy over our future reproductive health, agree that a woman seeking abortion should be provided with information on possible affects on her fertility and future pregnancies so we can decide for ourselves whether we want to accept those risks.
Please tweet this article!
- Tweet: Should We Care Whether Abortion Affects Fertility and Future Pregnancy Outcomes?
- Tweet: Any single abortion can increase the risk of developing Asherman syndrome or Pelvic Inflammatory Disease, either of which can lead to fertility issues
- Tweet: There is more than enough evidence to reasonably conclude that abortion can affect future pregnancies and women’s fertility
The post Should We Care Whether Abortion Affects Fertility and Future Pregnancy Outcomes? originally appeared at the Equal Rights Institute blog. Subscribe to our email list with the form below and get a FREE gift. Click here to learn more about our pro-life apologetics course, “Equipped for Life: A Fresh Approach to Conversations About Abortion.”






Please note: The goal of the comments section on this blog is simply and unambiguously to promote productive dialogue. We reserve the right to delete comments that are snarky, disrespectful, flagrantly uncharitable, offensive, or off-topic. If in doubt, read our Comments Policy.